Tearing Problems
Eyes that water too much are a very common concern for people of all ages. Excess tears normally occur in the wind, while chopping onions, and of course at a sad movie. But many people experience extra tearing much more frequently and without any obvious inciting cause – why is this?

There are several answers to this question, including blocked drainage of tears through the normal passageways, failure of the normal blinking pump, and even excessive eye dryness that sometimes stimulates extra tearing. We’ll cover each of these after a quick review of the normal way that tears flow. The medical term for excess tears is epiphora.
Normal Tear Flow
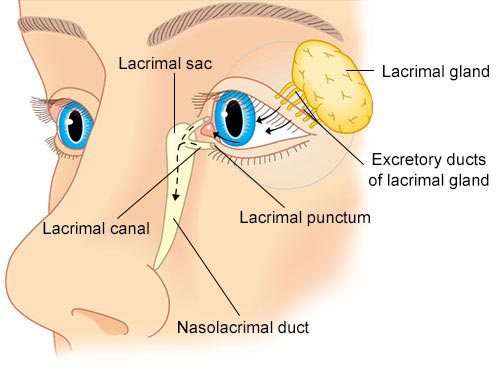
Normally, glands in the eye socket and eyelids make tears, which are then spread around by blinking to keep the eye always moist. Blinking pushes the tears inward toward the nose. Hidden in the inner corner of the upper and lower eyelids are a pair of drainage holes that connect to the nose with a set of tiny ducts. Thus, some tears normally flow into the nose with every blink, helping to keep the nose moist.
What Are the Most Common Causes of Tearing Problems?
We can all have watery eyes at times, such as a windy day that brings late spring pollen to our faces. But when you have abnormal amounts of tearing day in and day out, the typical causes are usually either blocked tear drainage ducts, problems with the eyelids, and dry eye, or some combination of all three. Here’s a little more about each of these reasons behind those watery eyes that are bothering you.
Blocked Tear Drainage Ducts
When you have a blocked tear duct, your tears can’t drain normally into your nose the way they always did before. This makes the eye tear abnormally: a watery eye. The blockage in the tear duct can be partial or complete. The lacrimal glands produce most of our tears. These glands are located inside the eye socket above each eye. Normally, tears flow from the lacrimal glands over the surface of the eye. These tears bathe and clean the eye, and then they drain into the tear ducts, first entering the puncta, located in the inside corners of your upper and lower eyelids.
From there, the eyelids have small canals that move tears to a sac where the lids are attached to the side of the nose, the lacrimal sac. The tears are pumped through the system by blinking and travel down another duct to drain into the nose. The body then reabsorbs them.
Blockage can occur anywhere in this elaborate drainage system, from the puncta in the corners of the eyelids to the nose. When blockage occurs, you’ll have watery eyes, and your eyes may be inflamed and more likely to develop infections.
Tear duct blockage is common in newborns (6% overall), but this usually resolves without any treatment during the first year of life. For older children and adults, tear ducts can become blocked by tear duct stones, inflammation, medications, infections, injury, sinus surgery, or very rarely, by a tumor.
Eyelid Problems
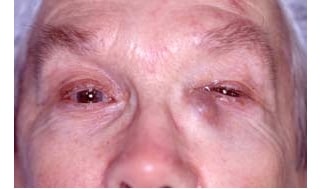
Ectropion is a condition where the lower eyelid turns outward, which leaves the inner eyelid surface exposed and prone to irritation. This happens usually in older people when the muscles under the eyes begin to weaken and the tendons stretch out. These muscles and tendons are responsible for keeping the eyelid tight against the eye. Ectropion can also be caused by facial paralysis, such as occurs with Bell’s palsy. It can be due to previous cosmetic eyelid surgery where the skin was removed from the lower eyelid.
Instead, some people will have a less obvious problem where the lower eyelid sags too low, exposing the delicate surface of the eye to the air and triggering reflex tearing to keep the eye wet. In many of these people, the loose eyelid also stops being able to effectively pump the tears into the tear drain. Consequently, the tears overflow onto the face.
Finally, the third group of people has upper eyelids that are very loose and open while they’re sleeping. The people awaken with watery, scratchy eyes. Many have sleep apnea, a closely associated problem, or habitually sleep face down.
Dry Eye
It can seem backward. How can eyes that are overly dry be watery? They can if you have “dry eye syndrome”, a condition where the eye produces too few tears or tears of an incorrect composition. The parched eye then asks the body to send more tears, which it does, but not efficiently and steadily enough to solve the underlying dryness. Hence many people experience irritated eyes that seem both dry and wet.
Dry eye can result from various problems. As we age, everyone’s tear production drops. This is especially true of women after menopause. Often, tear quality is diminished when the oil-making Meibomian glands are blocked because tears evaporate too quickly from the eye without the protection of the outer oil layer. There is yet another layer to the tears called mucus that helps them spread evenly across the eye and not “bead up” – certain diseases and injuries can reduce the mucus, causing dry eye symptoms. Finally, a variety of medications can also reduce tear production: antihistamines, diuretics, beta-blockers, sleeping pills, nerve medications, and pain relievers.
Dry eye really comes down to one of these (or a combination of) three problems:
- Lack of saltwater tears
- Dysfunctional Meibomian oil glands
- Dysfunctional mucus-producing glands
What Causes Watery Eyes?
Epiphora can result from a number of different causes. These include:
- The flow of tears is blocked
- Blinking doesn’t push tears to the inner eye corner
- Chronic Dryness or Irritation of the Eyes
At What Point Should I See a Doctor for My Watery Eyes?
Watery eyes can clear up on their own, especially for causes such as environmental issues. However, if the tearing is frequent throughout the day or goes on for weeks, the watery eyes can sometimes lead to more serious problems.
Blocked Tear Duct
The first thing that can go wrong is that the flow of tears from the eye to the nose gets blocked. The tears then have nowhere to go and they pool at the eye and run down the face. This can happen because the drainage holes close or because the ducts get blocked along the way to the nose. It can even happen in newborn babies when the final process of opening the ducts doesn’t occur on time (this affects about 1 in 20 newborns). Depending on when and where the blockage occurs, the treatment to solve the problem may be different.
For infants with tearing and mucus, pediatricians will often recommend a gentle massage at the inner corner of the eye to push the tears along and hopefully open the passage into the nose. If that doesn’t work by the first birthday, then an eye surgeon can pass a fine probe through the duct under anesthesia and usually solve the problem. Sometimes a temporary soft silicone plastic stent can be inserted to help as well.
For older children and adults with a closed tear drainage hole (the medical term is punctum), a minor surgery office procedure is often enough to open it and restore normal flow.
For older children and adults with blocked tear ducts deeper inside, things are a bit more complicated. Some of these people may have chronic or acute infections that cause redness, pus, or swelling in the inner corner of the eye, but many do not and only experience excess tears.
Nasal problems can also cause tearing since the normal tear duct drains into the nose. Polyps, tumors, sinus disease, and structural abnormalities in the nose can each contribute to excess tears. Depending on the actual problem, medication or outpatient surgery can be helpful.
What Are the Symptoms That Occur With a Blocked Tear Duct or Eyelid Problems That Cause Watery Eyes?
- Excessive, frequent tearing
- Redness of the sclera (the white part of the eye)
- Recurrent eye infection or inflammation
- Painful swelling near the inside corner of the eye
- Crusting of the eyelids
- Mucus or pus discharge from the lids and surface of the eye
- Blurred vision
Blinking Problem
The second thing that can go wrong is that, even though the drain is open, blinking fails to push the tears toward the inner corner. For these people, the problem is typically solved with outpatient day surgery to repair the integrity of the eyelids.
Age tends to loosen the tendons that keep the eyelids tautly snug against the eyeball. Often this permits the lower eyelid to drop down lower than normal and the tears pool at the lowest point, ready to drip down the cheek. The tendon at the outer corner can be tightened as outpatient day surgery, typically resolving the problem.
Any cause of facial paralysis, from Bell’s palsy to acoustic neuroma, can also reduce the efficiency of blinking, and create excess tearing. Again outpatient day surgery to improve eyelid closure and tension can help to solve the tearing problem.
Can Thyroid Eye Disease Cause Excessive Tearing?
Thyroid Eye Disease can cause the eyelids to widen and often reduces blinking. It can also cause swelling and irritation behind the eye and on the surface of the eye itself. All of this contributes to excess tearing. The proper treatment depends on the phase of the disease.
Dry Eye
This is counterintuitive. The third thing that causes excess tearing is chronic dryness or irritation of the eyes. Most people’s eyes become gradually drier as they age. This may not be an issue in humid climates, but in the arid West it is a huge problem. There are millions of dry eye sufferers in Colorado and the surrounding states, and the problem is even worse at high altitudes in the Rocky Mountains. Although the eyes may be chronically dry and irritated, they will still occasionally tear excessively when the body tries to reflexively wet them, sometimes misleading the person to think that the problem is wetness instead of dryness.
For people with dry eye syndrome, an eye specialist will usually prescribe artificial tears, and sometimes a series of other treatments that can help improve the quality and quantity of tears. See our summary. Outpatient eyelid surgery is not usually needed but can help certain people.

A similar cycle of dryness and wetness can happen to people after trauma or surgery near the eyes, especially after certain kinds of facial fracture repairs or cosmetic surgery under the eyes. Examination by a specialist will often disclose scarring of the lower eyelid that restricts proper blinking. Outpatient reconstructive surgery to restore eyelid position and movement will often help to resolve the problem.
Some people with sleep apnea develop a condition known as floppy eyelid syndrome that can affect the upper and lower eyelids. Since they often sleep face down, their floppy eyelids can flip inside out at night, exposing their eyes to the air and pillow. As a consequence, they often notice redness, irritation, and tearing in the mornings. CPAP machines and eye ointments may help, but for some people, outpatient eyelid surgery may be needed.
Watery Eyes Treatment
It is clear from the summary above that the treatment for excess tearing varies substantially depending on the cause. Evaluation by your optometrist or ophthalmologist may be sufficient to identify your problem and to start treatment, but you might be referred to an oculofacial plastic surgery specialist, such as Dr. Fante, for a more comprehensive evaluation. A specialist will examine the eyelids and surface of the eye, and will also usually probe and irrigate the tear ducts, and examine the nose to find all possible causes for excess tearing. For adults these tests can be easily accomplished in the office with minimal discomfort. However, for babies and small children, an evaluation (together with treatment) will be recommended under anesthesia.
What Can I Expect During My Evaluation for Watery Eyes?
When you see Dr. Fante, you’ll discuss your symptoms. When did the problem start? Did it change at some point? Has anything else changed with your medical situation?
Then they will examine your eyes and conduct a few tests. They’ll examine the inside of your nose to determine if your blockage is caused by structural issues in your nose. If they suspect blocked tear ducts, we may need other tests to find the location of your blockage. They might include:
- Tear drainage test — This test measures how quickly your tears are draining. One drop of a special dye is placed on the surface of each eye. If after five minutes most of the dye is still on the surface of your eye, it’s likely a blocked tear duct.
- Irrigation and probing — We may flush saline solution through your tear drainage system to check how well it’s functioning. Using anesthetics, we may insert a probe through the tiny drainage holes at the corner of your lid to check for blockages.
- Nasal examination – We may look at the structures inside the nose expertly using a gentle nasal endoscope to evaluate the outlet of the tear drainage system and to look for other possible causes of your tearing.
- Eye imaging tests — A contrast dye is passed from the puncta in the corner of your lid through your tear drainage system. Then an x-ray, CT scan, or MRI is taken to find the location of the blockage.
Surgery for Epiphora
As highlighted above, there are several different outpatient procedures used to solve the various different problems that cause excessive tearing. Depending on the patient and procedure, these are usually performed with conscious sedation or general anesthesia in an ambulatory surgery center or hospital. In some cases. surgery is needed to correct excessive tearing including upper/lower eyelid surgery or tear duct surgery.
Can Eyelid Surgery Correct Tearing Problems?
Eyelid Surgery is one method that Dr. Fante uses to treat tearing problems. In some patients, the eyelids are not tight enough to the eye, causing tears to drain improperly. The tearing system relies on the muscles of the eyelid to open and close the tear duct, which cannot happen if the eyelids are too loose. For blepharoplasty or eyelid surgeries, there is usually minimal pain but some swelling, bruising, and stitches are common. Most people can return to work or everyday life about a week after surgery.
Tear Duct Surgery for Watery Eyes
Outpatient day surgery is often necessary to restore tear flow through the normal channels or to bypass the blockage and deliver the tears to the nose, often with the placement of a temporary soft silicone plastic stent. The most commonly performed surgery is called DCR (for DacryoCystoRhinostomy). Dr. Fante is the co-author of the largest published series of DCR surgeries in America.
For the tear duct surgeries, there is also usually minimal pain. Many of these are accomplished using a nasal endoscope, and afterward, there is no swelling or bruising, but there is often a bloody nose for a few hours. People are able to return to work or everyday life within a few days. Other kinds of tear duct surgery are performed in the inner corner of the eye itself, and then there is often temporary swelling, bruising, and stitches that may delay return to work until a week after surgery.
Who is a Candidate for Tear Duct Surgery?
Because blocked tear ducts are among the most common causes of watery eyes, it may be necessary to perform what is called a dacryocystorhinostomy (DCR). In these procedures, Dr. Fante creates a new tear drain between your eyes and your nose.
This can be necessary if we’ve determined your tear ducts are blocked and there isn’t a non-invasive treatment option to correct the problem. These surgeries are far more common for adults than children with blocked tear ducts. In most cases, surgery won’t be pursued unless it is clear that non-surgical options such as warm compresses, massage, and antibiotics to clear an infection have been tried and proven unsuccessful for opening the blockage.
What Are the Risks With Tear Duct Surgery?
This is a commonly performed surgery that can be done using a small skin incision near the inner corner of the eye or using an endoscope to access the blocked area from the nose. Either way, it is an outpatient surgery and you go home the same day. Often a temporary stent or tube is placed inside the tear duct to help it heal well. The stent is typically removed in the office 6-12 weeks later. Tear duct surgery is successful 90-99% of the time, depending on the cause, and most people have no complications.
Uncommon risks of these surgeries include:
- Incomplete resolution of the tearing
- Scarring
- Displacement of the stent placed in the duct
- Excessive bleeding from the nose in first few days
- Infection
A thorough exam by your eye doctor will help you determine if your frequent tearing might be from an eyelid problem, a blocked tear drainage duct, or from dry eyes. You might even have all three. When you visit with Dr. Fante at the Fante Eye and Face Centre, we will work with your doctor to find the best solution(s) to your watery eyes, and we will be certain to make sure you understand the details.
What People Say About Us!
"“I had a wonderful experience with Dr Fante and his staff. My tearing problem is gone; plus, my eyes look so much better. Having a surgical procedure can, needless to say, be stressful, but Dr Fante’s skill combined with their outstanding client service made the whole process worry-free.”"
Click here to read more reviews.
Schedule a Consultation
If you are interested in treatment for excessive tearing problems in Denver, contact our office today! Call 303-839-1616 to schedule a consultation with facial plastic surgeon Dr. Robert Fante.